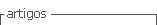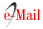Serviços Personalizados
Artigo
Links relacionados
Compartilhar
RGO.Revista Gaúcha de Odontologia (Online)
versão On-line ISSN 1981-8637
RGO, Rev. gaúch. odontol. (Online) vol.60 no.1 Porto Alegre Jan./Mar. 2012
CLÍNICO / CLINICAL
Recurrent Infection by varicella-zoster virus with facial scarring
Infecção recorrente pelo vírus varicela-zoster com sequelas cicatriciais na face
Maurício Malheiros BADARÓ I; Isabella da Silva Vieira MARQUES I; Maria Sueli da Silva KATAOKA I; Maria das Graças Rodrigues PINHEIRO II; Antônio Inácio ATHAYDE II; João de Jesus Viana PINHEIRO II
I Universidade Federal do Pará, Faculdade de Odontologia. Rua Augusto Corrêa, 1, Guamá, 66075-110, Belém, PA, Brasil
II Professora Mestre do Curso de Odontologia do Centro Universitário do Pará, Curso de Odontologia. Belém, PA, Brasil
ABSTRACT
Primary contact with the varicella-zoster virus occurs through varicella (chickenpox) and culminates with this virus entering the sensory nerves and remaining latent in the dorsal root ganglion. Transmission occurs by dissemination of infectious particles of the varicella-zoster virus by the aerosol released from nasopharyngeal secretions or skin lesions, or by direct contact with lesions. Herpes zoster occurs after clinically evident reactivation of the virus, affecting the whole distribution of the infected sensory nerve. When compared with primary infection, herpes zoster has a more severe character, requiring the use of pharmaceutical drugs. The cause of reactivation is unknown and may be associated with predisposing factors, such as age, stress or impaired immune system. This study reports a case of a patient who presented clinical manifestations compatible with varicella zoster infection exacerbated by the use of homemade remedies, resulting in a secondary infection and facial scarring.Indexing terms: Chickenpox. Herpes virus 3, human. Herpes zoster.
RESUMO
O contato primário com o vírus varicela-zoster ocorre na varicela (catapora), culminando com a transposição desse vírus para os nervos sensitivos, onde estabelece sua latência no gânglio espinhal dorsal. A transmissão ocorre por disseminação das partículas infecciosas do vírus varicela-zoster através de aerossóis liberados a partir de secreções do nasofaringe ou lesões cutâneas ou, ainda, pelo contato direto com lesões. O herpes-zoster clinicamente evidente ocorre após a reativação do vírus, com o envolvimento da distribuição do nervo sensitivo afetado. Quando comparado com a infecção primária, o herpes-zoster desenvolve um caráter de maior severidade, sendo sempre necessária a administração de uma terapêutica medicamentosa eficaz. A causa dessa reativação é desconhecida, podendo estar relacionada a fatores predisponentes como a faixa etária, estresse ou imunodeficiências. Neste trabalho relata-se um caso clínico em que a paciente apresentou manifestações clínicas condizentes com um quadro característico de infecção por varicela-zoster, complicado por uso de medicação caseira, resultando em infecção secundária e cicatrizes faciais.Termos de indexação: Varicela. Herpesvirus humano 3. Herpes zoster.
INTRODUCTION
The varicella-zoster virus (VZV) or human herpes virus type 3 (HHV3) is from the genus Varicellovirus, subfamily Alphahersvirinae and family Hespes-viridae. It is a double-stranded DNA virus with a diameter of 150 to 200 nm, has an icosahedral capsid and a lipoprotein envelope1. The transmission occurs via dissemination of infectious particles of the virus in aerosol released from nasopharyngeal secretions or skin lesions, or by direct contact with lesions of patients with chickenpox or herpes zoster1.
Primary infection by the virus varicella zoster results in chickenpox, followed by entrance of this virus in sensory nerves, where it remains latent in the dorsal root ganglion (DRG). When the virus reactivates, it becomes clinically evident by the development of herpes zoster, commonly known as shingles, and involves the distribution of the sensory nerve, from the trunk and head and neck region2-6.
When many branches of the trigeminal nerve are affected, it may result in unilateral oral, facial or ocular lesions. The main complications of herpes zoster include: postherpetic neuralgia, chronic lesions and changes in the central nervous system (CNS) and eyes4,7-8.
The reason for reactivation of the virus is unknown and may be related to predisposing factors, such as age (incidence increases proportionally with age), stress or immune system impairment stemming from tumors, acquired immunodeficiency syndrome (AIDS), autoimmune diseases and use of immunosuppressive drugs6-11.
The clinical characteristics of herpes zoster may be divided into three phases: prodromal, acute and chronic. During initial viral replication, active ganglionitis develops and results in neural necrosis and severe pain, responsible for the prodromal symptom of intense pain that precedes skin eruption in more than 90% of the cases. As the virus spreads along the nerve, pain worsens and manifests as burning, perforating, cutting, itching and/or discomfort on the dermatome, which is the area of the epithelium supplied by the affected sensory nerve. Before the onset of mucous and/or skin lesions, the patient may also experience malaise, headache and fever, in addition to the prodromal pain2-3.
The acute phase begins when clusters of blisters with erythematous base appear on the affected skin area. After some time, these blisters begin to pustulate and ulcerate. Crusts develop usually 7 days after blister onset, along the path of the affected sensory nerve, and ends at the midline. The rash in healthy individuals resolves within 2 or 3 weeks, leaving hypo- or hyperpigmentation marks. It is usually necessary and extremely important to work with a multidisciplinary team. The presence of lesions on the tip of the nose may indicate involvement of the nasociliary branch of the trigeminal nerve, with consequent ocular involvement. In these cases, intervention by an ophthalmologist is essential2.
The chronic phase is associated with postherpetic neuralgia, a denomination that refers to the pain that persists for more than 3 months after the initial manifestation on the skin. The pain is localized, continuous, throbbing, stabbing and burning. Most of the neuralgia subsides within one year2.
Shingles vaccine (Zostavax, Merck Sharp and Dohme, Haarlem, Netherlands) contains live, attenuated varicella-zoster virus. However, this vaccine is not 100% efficient. Zostavax contains a higher dosage of the vaccine virus than the chickenpox vaccine, and the results are considered good. The vaccine reduces the risk of developing herpes-zoster by 51%12-14.
The objective of the present study is to report the clinical case of a female patient aged 28 years who developed herpes-zoster.
CASE REPORT
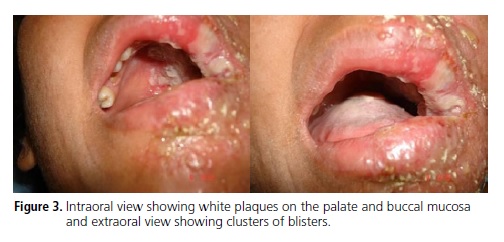
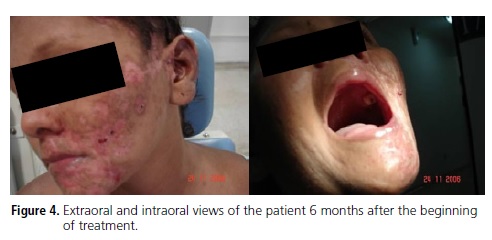
A 28-year old woman visited the Integrated Dental Clinic of the University Center of Pará (CESUPA) complaining of intense pain, toothache and left facial swelling (Figure 1). Her medical history included signs and symptoms of varicella zoster (chickenpox) in childhood. The patient reported that her initial symptoms were toothache and intense facial pain, burning and itching. Later, blisters appeared, which later became ulcers. The patient applied chicken fat with sulfur on the affected area. Extraoral signs included facial swelling with unilateral ulcers, blisters and pustules resulting from secondary infection, indicating involvement of the ophthalmic, maxillary and mandibular branches of the trigeminal nerve (Figure 2). Intraoral signs included white plaques and ulcers on the left palate, not crossing the midline, and left buccal mucosa (Figure 3). Based on the patient's clinical manifestations and medical history, the diagnosis was herpes-zoster. The prescribed treatment included a systemic antiviral drug, Penvir® (Fanciclovir, Sigma Pharma, Hortolândia, Brazil) at a dosage of two 125mg capsules at 8-hour intervals, a topical antiviral ointment, Penciclovir (Sigma Pharma, Hortolândia, Brazil), to be applied on the area at 2-hour intervals, and four 10mg sublingual tablets a day of ketorolac trometamol to relieve pain. The patient improved significantly with pharmacological treatment. The oral lesions disappeared after 80 (eighty) days and did not leave sequelae. However, although the skin in the affected area was still healing, it already presented hypo- and hyperpigmentation marks, probably stemming from the secondary infection. Facial swelling also resolved (Figure 4).
Before signing the free and informed consent form, the patient was informed that her pictures would only be used in scientific events and publications, all in accordance with the ethical principles set forth by the Declaration of Helsinki (2000).
DISCUSSION
The prevalence of varicella-zoster virus reactivation varies from 10 to 20%. It increases significantly after age 60 years with children representing less than 5% of the cases1-2,15. The present case occurred in a 28-yearold patient and so is not in the most affected age group according to the literature.
The main complaints of the patient were intense pain on the left side of the face and toothache in the affected region. The affected tissues were significantly swollen. These signs and symptoms were compatible with other published case reports1-3.
Although the disease can be perfectly diagnosed based on history and clinical picture, a classical ELISA assay can be used to confirm herpes zoster diagnosis by determining serum levels of IgG and IgM antibodies. IgG seroconversion or a significant increase in IgG titer/index between two paired samples, collected ten days apart, suggest recent infection16-19. During the medical history, the patient reported that she had already had chickenpox and that the present disease began with toothache, burning, itching and intense pain on the left side of the face. Later blisters appeared, which then became ulcers, manifestations described by Neville & Damm2.
Many opportunistic infections in human immunodeficiency virus (HIV)-infected patients are caused by the herpes group of viruses, presenting in the primary form or as recurrent herpes, especially in infected children. These viral infections increase both HIV dissemination and expression, debilitating the patient's immune response11. Therefore, it is important to determine if the patient with herpes zoster is infected by HIV. The patient of the present study is not infected with HIV11, contrary to other clinical cases reported in the literature5,9.
Involvement of the trigeminal nerve manifests by the formation of oral lesions in the mobile or attached mucosa. Often, the lesions extend to the midline and occur together with skin lesions that cover the affected quadrant. Oral lesions are white, opaque, range in diameter from 1 to 4 mm and proceed to form shallow ulcers. Additionally, teeth in the affected area may devitalize, there may be significant bone necrosis and permanent blindness may also ensue1-2. The clinical picture of the patient consisted of blisters and pustules on erythematous bases and considerable edema along the path of the left trigeminal nerve. There were also white plaques and ulcerations in the left palate and buccal mucosa, not crossing the midline, which corroborates other literature reports1-3,20-21. The homemade treatment used by the patient consisted of topical application of chicken fat mixed with sulfur. This homemade remedy hindered the healing process and probably caused the secondary infection present in the affected region, which culminated with the formation of fibrous scar tissue.
Initial treatment with appropriate antiviral drugs accelerates the healing process of the skin and mucosal lesions and reduces the duration of acute pain and postherpetic neuralgia. Once the skin lesions heal, neuralgia may become the worst aspect of the disease and it is usually hard to resolve it successfully2. This intense pain is usually treated with systemic and preferably topical painkillers but there are other methods available, such as physical medicine, psychotherapy, occupational therapy and anticonvulsant drugs (carbamazepine, phenytoin and sodium valproate)4. The treatment of the present case was based on the literature and consisted of systemic and topical antiviral drugs and painkillers. However, topical and systemic antiviral drugs, such as acyclovir and vidarabine, only relieve the symptoms of existing lesions; they do not exterminate the virus22.
It is important to point out that the amino acid L-lysine can significantly reduce herpes simplex virus 1 (HSV1) replication (herpes labialis) and healing time in animals. However, controlled clinical trials in larger samples are necessary to confirm its efficiency against herpes labialis and herpes zoster22.
Finally, it is extremely important to encourage all health professionals who have a negative or doubtful history of the disease or negative serology to receive immunization since, according to the literature, there has been a case of herpes zoster transmission from a patient with active lesions to a health provider. Therefore, occupational risks exist in healthcare facilities, and they need to be dealt with conscientiously and responsibly. The entire staff should be tested for varicella-zoster virus and the facility must have an effective vaccination program13-14,23-24.
CONCLUSION
The diagnosis of this disease is clinical. Therefore, the health professional needs to be attentive to its manifestations to diagnose it early and correctly and provide appropriate treatment.
Preventive measures should be used to prevent primary infection by the varicella-zoster virus. This may be achieved by implementing measures that prevent the exposure of patients to the virus, passive immunization (vaccine), active immunization or use of antiviral drugs after exposure.
When the clinical form of the disease is present, institution of treatment and patient education are extremely important to minimize or prevent sequelae, especially with regard to appropriate healing and preservation of the affected tissues.
Collaborators
MM BADARÓ, ISV MARQUES and MSS KATAOKA conceived and helped to write the article. MGR PINHEIRO and AI ATHAYDE treated the patient and helped to write the article. JJV PINHEIRO supervised the study and helped to write the article.
REFERENCES
1. Neto LK, Borba MG, Holderbaum RM, Figueiredo MAZ. Manifestações clínicas e tratamento da infecção recorrente pelo vírus varicela-zoster: relato de caso clínico. Rev Fac Odontol Univ Passo Fundo. 2003;8(2):20-3. [ Links ]
2. Neville BW, Damm DD. Patologia oral e maxilo-facial. 2ª ed. Rio de Janeiro: Guanabara Koogan; 2004.
3. Volkweis MR, Severo AF, Figueiredo MAS, Yurgel LS, Cherubini K. Herpes-zoster em paciente HIV positivo: relato de caso. Rev Fac Odontol Univ Passo Fundo. 2003;8(2):24-8.
4. Alvares FK, Siqueira SRDT, Okada M, Teixeira MJ, Siqueira JTT. Evaluation of the sensation in patients with trigeminal postherpetic neuralgia. J Oral Pathol Med. 2007;36(6):347-50.
5. Abdul Latheef EN, Pavithran K. Herpes zoster: a clinical study in 205 patients. Indian J Dermatol. 2011;56(5):529-32.
6. Cebrián-Cuenca AM, Díez-Domingo J, San-Martín-Rodríguez M, Puig-Barberá J, Navarro-Pérez J. Epidemiology and cost of herpes zoster and postherpetic neuralgia among patients treated in primary care centres in the Valencian community of Spain. BMC Infect Dis. 2011;11(1):1-12.
7. Opstelten W, van Loon AM, Schuller M, van Wijck AJ, van Essen GA, Moons KG, et al. Clinical diagnosis of herpes-zoster in family practice. Ann Fam Med. 2007;5(4):305-9.
8. Neves OS, Facó MMM, Sallum AME, Campos LMA, Rossi Júnior A, Silva CAA. Herpes-zoster em pacientes com lúpus eritematoso sistêmico juvenil. Rev Bras Reumatol. 2007;47(2):135-9.
9. Reis HL, Cavalcante FS, Santos KR, Passos MR, Ferreira DC. Herpes zoster as a sign of AIDS and nonadherence to antiretroviral therapy: a case report. Clinics. 2011;66(12):2179-81.
10. Gonzaga HFS, Jorge MA, Gonzaga LHS, Barbosa CAA, Chaves MD. Systemic and oral alterations in brazilian patients with cutaneous herpes-zoster. Braz Dent J. 2002;13(1):49-52.
11. Silva RA, Lopes FF, Barreto AM. Estudo clínico das manifestações orais da síndrome de imunodeficiência adquirida pediátrica. RGO - Rev Gaúcha Odontol. 2002;50(1):7-11.
12. Harpaz R, Ortega-Sanchez IR, Seward JF. Prevention of herpes-zoster: recommendations o the Advisory Committee on Immunization Practices (ACIP). MMWR Recomm Rep. 2008;57(28):779.
13. Shapiro M, Kvern B, Watson P, Guenther L, McElhaney J, McGeer A. Update on herpes zoster vaccination: a family practitioner's guide. Can Fam Physician. 2011;57(10):1127-31.
14. Oxman MN. Zoster vaccine: current status and future prospects. Clin Infect Dis. 2010;51(2):197-213.
15. Johnson RW, Dworkin RH. Treatment of herpes-zoster and postherpetic neuralgia. BMJ. 2003;326:748-50.
16. Costa MRM, Ramos CS, Monteiro TAF. Prevalência de IgG do vírus varicela-zoster (VVZ) em indígenas da tribo araweté, em Altamira, Pará, de Janeiro-Fevereiro de 2001. Rev Para Med. 2006;20(4):23-8.
17. Reis AD, Pannuti CS, Souza VAUF. Prevalência de anticorpos para o vírus da varicela-zoster em adultos jovens de diferentes regiões climáticas brasileiras. Rev Soc Brás Med Trop. 2003;36(3):317- 20.
18. Arvin AM, Koropchak CM. Immunoglobulins M and G to varicellazoster virus measured by solid-phase radioimmunoassay: antibody responses to varicella and herpes zoster infections. J Clin Microbiol. 1980;12(3):367-74.
19. Barak M, Weinberger R. Outcome of IgM and Ig G seropositive cases of varicella zoster in pregnancy. J Reprod Med. 2004;49(1):38-40.
20. Alchorne MA, Alchorne AO. Infecções cutâneas virais. In: Cucé LM, Festa Neto C. Manual de dermatologia. 2ª ed. São Paulo: Atheneu; 2001. p. 209-11.
21. Silva S, Salomone C. Herpes zóster y neuralgia posherpética. Rev Chil Dematol. 2005;21(1):38-46.
22. Pedrazini MC, Cury PR, Araujo VC, Wassall T. Efeito da lisina na incidência e duração das lesões de herpes labial recorrente. RGO - Rev Gaúcha Odontol. 2007;55(1):7-10.
23. Ku CH, Liu YT, Christiani DC. Case report: occupationally related recurrent varicella (chickenpox) in a hospital nurse. Environ Health Perspect. 2005;13(10):1373-5.
24. Carvalho ES, Martins RM. Varicela: aspectos clínicos e prevenção. J Pediat. 1999;75(1):126-34.
 Correspondence to:
Correspondence to:
JCV RIBEIRO
e-mail: jcarlosvr@gmail.com
Received on: 22/11/2010
Final version resubmitted on: 9/4/2011
Approved on: 28/5/2012