Serviços Personalizados
Artigo
Links relacionados
Compartilhar
RSBO (Online)
versão On-line ISSN 1984-5685
RSBO (Online) vol.12 no.3 Joinville Jul./Set. 2015
ORIGINAL RESEARCH ARTICLE
Oral health status of patients with special needs from a rehabilitation association in Curitiba (PR, Brazil)
Cecim Calixto JuniorI; Marilisa Carneiro Leão GabardoI; João Armando BrancherI; Mariana DalledoneI; Tatiana LuzziI; Eduardo PizzattoI
I Program of Master Science in Clinical Dentistry, Positivo University – Curitiba – Paraná – Brazil
ABSTRACT
Introduction:Patients with special needs commonly show significant systemic and oral diseases. Objective:We carried out a survey on the oral health status from individuals with special needs of Associação Paranaense de Reabilitação (APR), in Curitiba, PR, Brazil. Material and methods: Clinical oral examination was performed and a specific questionnaire was applied to 87 individuals, aged from 5 to 14 years-old. Results: The mean age average was 9 yearsold, and 57.5% were males. The mean DMFT was 1.4, and 54% of the sample showed DMFT = zero. The oral health status from the studied sample was similar to that found in the same age group of the general population. Conclusion: We indicate that strategies for controlling oral health diseases tailored for this group must be stimulated, once the vulnerability is present.
Keywords: oral health; epidemiology; people with special needs.
Introduction
The patient with special needs is considered as every individual that has either simple or complex physical, organic, intellectual, social, emotional changes; of acute or chronic nature; and requires special education and additional instructions, temporarily or permanently 27.
The fact that an individual has special needs somehow implies limiting conditions, whose origin can be congenital or acquired over life 5. In 2010, 23.9% of the population claimed to have some type of disability, with higher concentration in urban areas 19. Evidences indicate that the highest concentration of people with special needs (PSNs) occurs in groups with unfavorable conditions, such those with low income 13,39.
PSNs commonly present systemic and oral characteristics. The most prevalent oral disease is dental caries and periodontal disease 10,20,22,24,34,37,40.
There are indications that the institutionalized PSNs may be at increased risk of caries development compared to non-institutionalized 14,18. More compromising disability cases are found more often in specialized institutions, which coincide with the fact that these individuals have higher rates of diseases 22,34. These finding are caused by common set of factors such as poor oral hygiene 10, use of psychoactive drugs 10 and dietary patterns 7,30, which increase the risk of developing diseases.
In different locations worldwide, studies highlight the need for improvements in organizational strategies to strengthen preventive measures, together with the rehabilitative interventions for this population, supported by changes in the health policies aimed at expanding the service to these patients 1,13,24,34,35,37.
Early dental care of PSNs and multidisciplinary care have an important role, but challenges the dentist according to the skills 7-9,23-25,32.
In Brazilian population, the difficulty lies in having few specialized centers to provide assistance to these patients and the limited number of qualified professionals for the treatment, either in public or private practice 16,31.
One should also consider the complexity of the answers that can be given by families concerning the problems presented by these children 11. The family motivation and disinterest may arise in relation to oral health of PSNs 36, as well as the lack of oral health knowledge and attitudes of professionals for the education of patients with special needs 28.
The educational process in dentistry, attempting to change the behavior, is essent ial for the maintenance, acquisition, and promotion of selfcare in oral health 36,38, is now not relevant, and hence the restorative treatment is necessary. In this context and as a result, the quality of life associated with oral health is impacted 17, theme addressed in the context of PSNs 32.
This study aimed to evaluate the oral health status of a group of PSNs from the Paranaense Association of Rehabilitation (APR), at the city of Curitiba, Brazil.
Material and methods
This cross-sectional study with non-probabilistic sample was composed of students from an institution (Curitiba, Brazil). Inclusion criteria comprised the age range of 5 to14 years-old and prior signing of the Free and Clarified Consent Form by the parent/legal guardian. Eight-seven of 205 individuals participated in the study. This study was submitted and approved by the Ethical Committee in Research of Positivo University under protocol no. #155/2009.
The following variables were evaluated: age, gender, periodontal disease, soft tissue alteration, occlusion, fluorosis, and dental caries.
The intraoral clinical examination followed the standards recommended by the World Health Organization26. Periodontal disease was measured through the identification of gingival changes and recorded as absent or present. The same classifications were possible for the change of soft tissue and the presence of visible plaque. Occlusion was classified as normal, mild, moderate, or severe malocclusion. For fluorosis, the possibilities were: normal, questionable, very mild, mild, moderate or severe.
The examinations were performed by calibrated examiners, under artificial light, with wooden spatula, with the patient sat and the examiner stood up.
The collected data were recorded, tabulated, and analyzed through Statistica 8.0 software.
Results
The result of the Kappa test to evaluate the interexaminer agreement was 0.86.
The sample mean age was 9 years (SD = 2.5).
Male individuals accounted for 57.5% of the sample.
With regard to the oral status evaluated, the gingival changes are shown in 6.9% of examined PSN, with the presence of visible plaque in 57.5%, while the soft tissue changes were present in 4.6% of cases. Occlusal problems were found in over 50% of the examined according to standard classifications (47.1%) in mild (36.8%) and moderate or severe malocclusion (16.1%).
Fluorosis represented 3.3% of subjects, with equitable distribution rate of 1.1% between mild, moderate and severe scores.
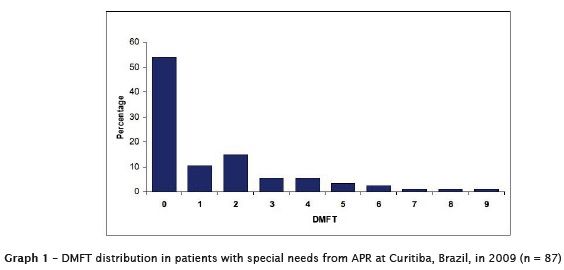
The average DMFT value was 1.4 (SD = 2), and 54% of the examined had DMFT = zero. The distribution of DMFT values can be observed in graph 1.
Discussion
The literature suggests that the most prevalent oral disease in patients with special needs is caries and periodontal disease 10,22,24,34,37,40. However, the results of this study did not indicate a significant proportion of these diseases, because the estimates of oral conditions were close to those of the same age groups of the population considered as "normal" 3,4.
With regard to caries, the DMFT average (1.4) was lower than values found in the literature ranging from 2.27 15, 2.41 20, 2.48 24, 3 14 to 5.4 34. In a recent study with Indian PSNs caries was found in 79.2% of respondents 37.
This study did not set aimed to compare PSNs with other groups of individuals, but considering DMFT variable, the mean value (1.4) was close to the average for 12-year-old children in the city Curitiba, in 2010, whose value was 1.53 4. However, we highlight that possible differences in the methodology of the studies can lead to variation in the results.
The high consumption of drugs among PSNs is considered the source for increased risk of caries development 10, although there are contradictions 15. The institutionalization was also considered a risk factor 14,18,22,34. Recognition of the role of poor oral hygiene in triggering problems 10, especially in those individuals with higher psychomotor difficulties, is a critical issue.
The low frequency of gingival changes found in this study corroborates previous findings 6, but contradicts other recent findings, in which healthy periodontal condition was not found in any participant 37. The Brazilian epidemiological survey conducted in 2003 pointed to a rate slightly higher than 6% of gingival changes in 5-year-old children 3.
The soft tissue changes are also highlighted with many types 33. In this present study, a low prevalence of this disease was seen.
Concerning to malocclusion, these are often detected in patients with special needs, especially in Down syndrome as a result of muscle hypotonia and macroglossia 31,37. These findings of this study corroborate the literature and the data of the 5 to 12-year-old Brazilian population 3,4.
Several studies have been conducted to achieve knowledge on oral health status of PSNs seeking the implementation of programs and educational/ preventive actions 1,13,24,25,34,35. Also, other points have to be overcome, such as lack of training in handling these patients 2,16,23,31, the lack of multidisciplinary care 7-9,23-25,32,35, and the need to instruct the parents/guardians to perform effective oral hygiene 9,21,32,38.
In Brazil the specialty of Dentistry for Patients with Special Needs was regulated by Federal Council of Dentistry in December 2001 12. This particular training is of utmost importance, since the dentists attending children with special needs report experiencing difficulties in describing the real demands of these patients 16.
It must be considered that the high prevalence of dental caries admittedly has impacts on the quality of life of all people 17, likely PSNs 32.
Further studies are necessary to clarify the association of other variables, e.g. socioeconomic and oral health-related quality of life, with the oral health status of PSNs.
Conclusion
Based on the results obtained in this study, it is concluded that PSNs, in general, showed good oral health status, with data similar to those found in the general population. Efforts should be encouraged to seek the proper oral health of these individuals because of their vulnerability.
References
1. Abreu MHNG, Castilho LS, Resende VL. Assistência odontológica a indivíduos portadores de deficiências: o caso da Associação Mineira de Reabilitação e Escola Estadual João Moreira Salles. Arq Odontol. 2001;37(2):153-61. [ Links ]
2. Ahmad MS, Razak IA, Bor romeo GL. Undergraduate education in special needs dentistry in malaysian and Australian dental schools. J Dent Educ. 2014;78(8):1154-61.
3. Brasil. Ministério da Saúde. Secretaria de Atenção à Saúde. Departamento de Atenção Básica. Projeto SB Brasil 2003: condições de saúde bucal da população brasileira 2002-2003: resultados principais. Ministério da Saúde; 2004. 68 p.
4. Brasil. Ministério da Saúde. Secretaria de Atenção à Saúde. Secretaria de Vigilância em Saúde. SB Brasil 2010: Pesquisa Nacional de Saúde Bucal: resultados principais. Ministério da Saúde; 2012. 116 p.
5. Brugnera Jr A. Conceituando o paciente com necessidades especiais. In: Varellis MLZ. O paciente com necessidades especiais na Odontologia. Manual prático. São Paulo: Livraria Santos; 2005. p. 3-12.
6. Campos JADB, Giro EMA, Orrico SRP, Oliveira APC, Lorena SM. Correlação entre a prevalência de cárie e a utilização de medicamentos em pacientes com necessidades especiais institucionalizados e não institucionalizados. Salusvita. 2006;25(1):35-42.
7. Campos JADB, Zuanon ACC, Giro EMA, Abreue- Lima FCB. Padrão de alimentação do paciente com necessidades especiais e seu reflexo na cavidade bucal. JBP Rev Ibero-am Odontopediatr Odontol. 2005;8(42):127-34.
8. Cançado Figueiredo M, Carvalho e Silva SR, Preto Guimarães F, Araujo VP. Perfil de pacientes con necesidades especiales. Bol Assoc Argent Odontol Niños. 2003;32(1):8-11.
9. Carvalho ACP, Figueira LCG, Utumi ER, Oliveira CO, Oliveira LPN, Pedron IG. Considerações no tratamento odontológico e periodontal do paciente deficiente visual. Rev Odontol Bras Central. 2010;19(49):97-100.
10. Carvalho EMC, Araújo RPC. A saúde bucal em portadores de transtornos mentais e comportamentais. Pesq Bras Odontoped Clín Integr. 2004;4(1):65-75.
11. Ciênc Saúde Coletiva. 2003 Jan [cited 2014 Sep 12]; 8(3):830-1. Available from: URL: http://www.scielosp.org/scielo.php?script=sci_ arttext&pid=S1413-81232003000300018&lng =en.
12. Conselho Federal de Odontologia – CFO. Resolução CFO-22/2001. Baixa normas sobre anúncio e exercício das especialidades odontológicas e sobre cursos de especialização revogando as redações do Capítulo VIII, Título I; Capítulo I, II e III, Título III, das normas aprovadas pela Resolução CFO-185/93, alterada pela Resolução CFO-198/95. CFO; 2001. 27 p.
13. Costa MLP, Costa MABT, Pereira MF. Perfil clínico-epidemiológico de pacientes com paralisia cerebral assistidos em um centro de odontologia do Distrito Federal. Comun Ciênc Saúde. 2007;18(2):129-39.
14. De Jongh AD, van Houtem C, van der Schoof M, Resida G, Broers D. Oral health status, treatment needs, and obstacles to dental care among noninstitutionalized children with severe mental disabilities in The Netherlands. Spec Care Dentist. 2008;28(3):111-5.
15. Donnel DO, Sheiham A, Wai YK. Dental findings in 4-, 14-, and 25- to 35- year-old Hong Kong residents with mental and physical disabilities. Spec Care Dentist. 2002;22(6):231-4.
16. Fonseca ALA, Azzalis LA, Fonseca FLA, Botazzo C. Análise qualitativa das percepções de cirurgiõesdentistas envolvidos nos atendimentos de pacientes com necessidades especiais de serviços públicos municipais. Rev Bras Crescimento Desenvolv Hum. 2010;20(2):208-16.
17. Gabardo MCL, Moysés ST, Moysés S. Autopercepção de saúde bucal conforme o Perfil de Impacto da Saúde Bucal (OHIP) e fatores associados: revisão sistemática. Rev Panam Salud Publica. 2013;33(6):439-45.
18. Giro EMA, Orrico SRP, Campos JADB, Lorena SM, Cortez LMS. Prevalência de cárie em pacientes com necessidades especiais institucionalizados ou não-institucionalizados: consumo de carboidratos simples. Rev Odontol Unesp. 2004;33(2):75-9.
19. Instituto Brasileiro de Geografia e Estatística – IBGE. Censo demográfico 2010. Características gerais da população, religião e pessoas com deficiência. Rio de Janeiro; 2012. 215 p.
20. Jain M, Mathur A, Kumar S, Dagli RJ, Duraiswamy P, Kulkarni S. Dentition status and treatment needs among children with impaired hearing attending a special school for the deaf and mute in Udaipur, India. J Oral Science. 2008;50(2):161-5.
21. Marcelino G, Parrilha VA. Educação em saúde bucal para mães de crianças especiais: um espaço para a prática dos profissionais de enfermagem. Cogitare Enferm. 2007;12(1):37-43.
22. Mitsea AG, Karidis AG, Donta-Bakoyianni C, Spyropoulos ND. Oral health status in Greek children and teenagers, with disabilities. J Clin Pediatr Dent. 2001;26(1):111-8.
23. Moraes ABA, Batista CG, Lombardo I, Horino LE, Rolim GS. Verbalizações de alunos de Odontologia sobre a inclusão social de pessoas com deficiência. Psicologia em Estudo. 2006;11(3): 607-15.
24. Oliveira AC, Czeresnia D, Paiva SM, Campos MR, Ferreira EF. Uso de serviços odontológicos por pacientes com síndrome de Down. Rev Saúde Pública. 2008;42(4):693-9.
25. Oliveira ALBM, Giro EMA. Importância da abordagem precoce no tratamento odontológico de pacientes com necessidades especiais. Odonto. 2011;19(38):45-51.
26. Organização Mundial da Saúde – OMS. Levantamentos básicos em saúde bucal. 4. ed. São Paulo: Santos; 1999. 66 p.
27. Peres AS, Peres SHCS, Silva RHA. Atendimento a pacientes especiais: reflexão sobre aspectos éticos e legais. Rev Fac Odontol Lins. 2005;17(1):49-53.
28. Pomarico L, Souza IPR, Tura LFR. Oral health profile of education and health professionals attending handicapped children. Pesqui Odonto Bras. 2003;17(1):11-6.
29. Rao DB, Hedge AM, Munshi AK. Caries prevalence amongst handicapped children of South Canara district, Kamataka. J Indian Soc Pedod Prev Dent. 2001;19(2):67-73.
30. Resende VLS, Castilho LS, Viegas CMS, Soares MA. Fatores de risco para a cárie em dentes decíduos de portadores de necessidades especiais. Pesq Bras Odontoped Clín Integr. 2007;7(2):111-7.
31. Santangelo CN, Gomes DP, Vilela LO, Deus TS, Vilela VO, Santos EM. Avaliação das características bucais de pacientes portadores de síndrome de Down da Apae de Mogi das Cruzes – SP. Editorial ConScientiae Saúde. 2008;7(1):29-34.
32. Santos BMO, Aquino DJN, Pires-de Sousa FCP, Almeida GL, Garcia LFR. Assistência odontológica a portadores de necessidades especiais sob a ótica dos cuidadores. Ciênc Odontol Bras. 2009;12(2): 49-56.
33. Santos GG, Marcucci G. Contribuição para o estudo da prevalência das alterações dos tecidos moles da boca em pacientes especiais. Rev Odontol Univ São Paulo. 1989;3(2):357-62.
34. Shyama M, Al-Mutawa SA, Morris RE, Sugathan T, Honkala E. Dental caries experience of disabled children and young adults in Kuwait. Community Dent Health. 2001;18(3):181-6.
35. Silva OMP, Panhoca L, Blachman IT. Os pacientes portadores de necessidades especiais: revisando os conceitos de incapacidade, deficiência e desvantagem. Salusvita. 2004;23(1):109-16.
36. Silva ZCM, Pagnoncelli SD, Weber JBB, Fritscher AMG. Avaliação do perfil dos pacientes com necessidades especiais da Clínica de Odontopediatria da Faculdade de Odontologia da PUCRS. Rev Odonto Ciênc. 2005;20(50):313-8.
37. Solanki J, Gupta S, Arya A. Dental caries and periodontal status of mentally handicapped institutilized children. J Clin Diagn Res. 2014;8(7): ZC25-7.
38. Tomita NE, Fagote BR. Programa educativo em saúde bucal para pacientes especiais. Odontologia e Sociedade. 1999;1(1/2):45-50.
39. Waldman HB, Perlman SP. Children with special health care needs: results of a national survey. J Dent Child. 2006;73(1):57-62.
40. Whyman RA, Treasure ET, Brown RH, MacFadyen EE. The oral health of long-term residents of a hospital for the intellectually handicapped and psychiatrically ill. N Z Dent J. 1995;91(404):49-56.
 Corresponding author:
Corresponding author:
Eduardo Pizzatto
Rua Prof. Pedro Viriato Parigot de Souza, 5.300 – Campo Comprido
CEP 81280-330 – Curitiba – PR – Brasil
E-mail: epizzatto@up.edu.br
Received for publication: May 14, 2015
Accepted for publication: July 13, 2015