Services on Demand
Article
Related links
Share
Brazilian Journal of Oral Sciences
On-line version ISSN 1677-3225
Braz. J. Oral Sci. vol.10 n.3 Piracicaba Jul./Sep. 2011
ORIGINAL ARTICLE
Fracture strength of ceramic brackets submitted to archwire torsional strain
Fernando Rayes ManhãesII;Rosilene DivinoI; Adriana Simone LucatoIII; Sílvia Amélia Scudeler VedovelloIII; Cristian CorreaII; Heloísa Cristina ValdrighIII
I Undergraduate student in Dentistry, Fundação Hermínio Ometto-UNIARARAS, Araras, SP, Brazil
II DDS, Master student in Orthodontics, Fundação Hermínio Ometto-UNIARARAS, Araras, SP, Brazil
III PhD, Professor in Orthodontics, Fundação Hermínio Ometto-UNIARARAS, Araras, SP, Brazil
ABSTRACT
Aim: To evaluate the fracture strength of ceramic brackets submitted to archwire torsional strain. Methods: Different types of maxillary central incisor ceramic brackets from four different commercial brands, Roth prescription (0.022" x 0.028"), were evaluated, namely: Mystique (GAC), InVu (TP Orthodontics), Clarity (3M Unitek) and Luxi II (RMO Ortohodontics). To evaluate the fracture strength, 0.019"x 0.025" stainless steel orthodontic wires were inserted into the bracket channels and submitted to torsion until they fractured. Results: The InVu brackets showed a significantly higher fracture strength than the other brackets (p<0.05), which did not differ significantly among them (p>0.05). Conclusions: Among the brackets tested, the traditional ceramic bracket InVu showed the highest fracture strength, while the Luxi II bracket, obtained the lowest value.
Keywords: braces, ceramics, orthodontics, biomechanics.
Introduction
As patients who seek orthodontic treatment attribute great importance to esthetics, particularly the growing number of adult patients, esthetic brackets has been increasingly used instead of metal brackets. Among the esthetic brackets, those made of polycarbonate and ceramic are outstanding at present1. Ceramic brackets are more frequently used than those made of polycarbonate, due to their better physical and mechanical properties2, better color stability, esthetics and wear resistance than polycarbonate brackets. Nevertheless, ceramic brackets are more friable, generate more friction with the orthodontic wire, and may cause enamel wear in the antagonist tooth when coming into contact with it3-5.
Ceramic brackets are composed of aluminum oxide (Al2O3) and may be monocrystalline (a single aluminum oxide crystal) or polycrystalline (several aluminum oxide crystals fused at high temperatures)6. The major difference between polycrystalline and monocrystalline brackets is translucence. Monocrystalline brackets are more translucent than the polycrystalline type, which tend to be opaque4. In addition, monocrystalline ceramic brackets are more resistant to fracture than the polycrystalline type due to the greater tensile strength of the monocrystalline alumina7. Nevertheless, polycrystalline brackets are more frequently used because they are easier to produce and have a lower cost1.
Over the last few years, studies have been conducted to compare the fracture strength of ceramic brackets during second and third order activations, as ceramic brackets present high friability and low tensile strength8-9. The moment of torque normally applied to anterior teeth is one of the causes of ceramic bracket fractures10-11. The site of major ceramic bracket fracture is at the base of the winglets, probably because this area concentrates a greater deal of stress12 and is the most handled area by the orthodontist when inserting and removing wires and accessories, thus creating microscratches that contribute to the formation and propagation of cracks12-14 and increase bracket susceptibility to fracture1,15. Thus, the aim of this study was to evaluate the fracture strength of four different types of polycrystalline ceramic brackets submitted to archwire torsion or torque.
Material and methods
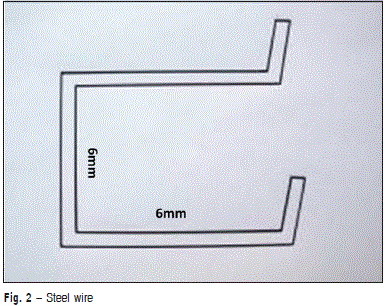
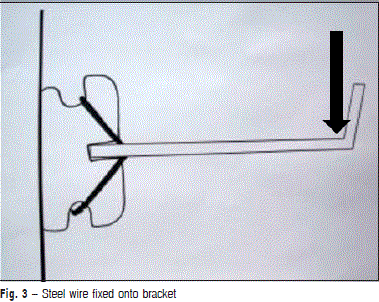
Forty maxillary right central incisor brackets, Roth prescription (0.022" x 0.028"), of four different commercial brands (n=10) were evaluated. Among the brackets (Figure 1), there were four polycrystalline types, being traditional ceramic semi-twin Mystique (GAC International, Bohemia, NY, USA), traditional ceramic twin InVu (TP Orthodontics, LaPorte, IN, USA), ceramic semi-twin with gold-reinforced channel Luxi II (Rocky Mountain Orthodontics, Denver, CO) and ceramic twin with stainless steel-reinforced channel Clarity (3M Unitek, St. Paul, MN, USA). Each bracket was fixed in a PVC cylinder (Tigre do Brasil, Joinville, SC, Brazil) filled under vibration with chemically activated acrylic resin (Jet Set; Clássico Artigos Odontológicos Ltda., São Paulo, SP, Brazil), at the sand stage, proportioned and prepared in accordance with the manufacturer's recommendations. After polymerization and smoothing the resin surface with 220-grit silicon carbide abrasive papers (Norton S.A., São Paulo, SP, Brazil), the brackets were fixed onto the surface of the cylinders using cyanoacrylate adhesive (Super Bonder, Loctite, São Bernardo do Campo, SP, Brazil). Forty segments of 0.019" x 0.025" 30-mm-long stainless steel (GAC) arches were bent into U-shapes with 6 mm of width and height, using 139 pliers (Dentaurum, Ispringen, Germany). The bends were made in juxtaposition to the bracket wings. A vertical bend was made at a distance of 6 mm from the bracket so that it could be used as a support for the test machine chisel (Figure 2). This distance of 6 mm from the bracket up to the point of support of force was used because it is the mean inter-bracket distance. For the mechanical test, the wire was inserted into the bracket channel through the base of the "U" pre-contoured with 0.019" x 0.025" wire and fixed with 0.008" tying wire (Figure 3).

Mechanical Test
The PVC cylinder (Tigre do Brasil) was adapted to a universal testing machine (Instron 4411) so that the cervical winglets were positioned facing downwards, and so that the machine chisel would be supported on the wire rods, where the chisel had the vertical bends of the wire as a stop so that it would not slide during the test. In this test, the wire was pushed downwards by the universal test machine chisel, simulating a vestibular torque, this being the reason why the bracket was positioned with the cervical winglets facing down. The test was performed at a crosshead speed of 1.0 mm/min until bracket fracture occurred. Data (kgF) were transformed into g·mm and submitted to ANOVA and Tukey's test at a level of significance of 5%.
Results
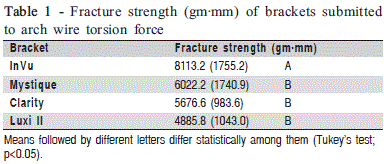
One-way ANOVA showed that there was significant difference for the fracture strength of brackets submitted to torsion strain (p<0.001). Among the polycrystalline brackets, the highest fracture strength (g·mm) was obtained with the traditional ceramic InVu (8113,2 ± 1755,2 g·mm) followed in a decreasing order by the traditional ceramic Mystique (6022.2 ± 1740.9 g·mm), ceramic with metal channel Clarity (5676.6 ± 983.6 g·mm) and ceramic with gold channel Luxi II (4885.8 ± 1043.0 g·mm). The results of Tukey's test (Table 1) revealed that the InVu brackets presented a statistically higher fracture strength (p<0.05) than the Mystique, Clarity and Luxi II brackets, which did not differ significantly among them (p>0.05).
Discussion
TEvaluation of the fracture strength of ceramic brackets submitted to archwire torsion strain was held due to the high friability and low tensile strength of ceramic brackets, particularly during the second and third order activations8-9.
Design and manufacturing process are factors that determine the strength of ceramic brackets, and the channel and winglet designs are critical for the strength of the accessory. The winglets may easily fracture due to the high flexural strength exerted by the rectangular arches, and this process is facilitated by the presence of defects on the surface and within the ceramic brackets, which may lead to crack propagation when the bracket it submitted to the action of forces14.
In the present study, InVu brackets presented a significantly higher fracture strength than the Mystique, Clarity and Luxi II brackets (p<0.05), which did not differ from each other (p>0.05). These results corroborate those of a previous study7, in which the twin ceramic brackets InVu presented higher fracture strength of the winglets under traction than the twin ceramic brackets Clarity and semitwin Luxi II brackets. Already Nishio11, testing the strength of esthetic brackets with torsion forces of the arch, found that the Clarity brackets showed higher fracture resistance to the brackets Luxi II.
One of the factors responsible for the higher fracture strength of the twin ceramic bracket InVu may be due to its fabrication method. For these brackets, the fabrication process is molding by injection, which makes it possible to obtain uniform surfaces with fewer irregularities when compared with brackets fabricated by the machining method16. Injection molded brackets have a smoother finish than machined brackets, thus reducing the number of surface defects14. Thus, these brackets have greater fracture strength under traction when compared with twin ceramic brackets fabricated by machining, which show damage and defects caused by the equipment during fabrication, and serve as foci for fractures12,13.
The lowest fracture strength was obtained with the goldreinforced ceramic bracket Luxi II (RMO, Orthodontics). This may have occurred due to the thinness of the wings in the occlusogingival and buccolingual directions, when compared with the other ceramic brackets. Another characteristic of the Luxi II brackets is their rougher surface morphology, making the ceramic material more susceptible to crack propagation and fracture7,12. This might have occurred as a result of the method of fabricating this bracket, capable of promoting defects and roughness on the surface of these materials, and significantly reducing the ceramic fracture strength5,13,17.
Of the brackets reinforced with a metal channel, gold reinforcement Luxi II was less efficient than stainless steel reinforcement Clarity, though without statistically significant difference. One of the hypotheses for this result was raised in a previous scanning electron microscopy study11, which stated that the sealant material between the gold channel and the bracket appeared to be thicker than the sealant material between the stainless steel channel and bracket. This sealant material could affect the channel rigidity and fracture strength.
The traditional semi-twin ceramic bracket Mystique presented the second highest fracture strength, but without statistically significant difference from the Clarity and Luxi II brackets. This might have occurred due to the morphological characteristics of the brackets, as in the semitwin brackets the mesial and distal winglets could be seen as a single unit. In this bracket configuration, there is a point of ceramic connected to the winglets, which in turn, has the effect of a transverse stabilizer. The mesial and distal winglets are not designed independently of the bracket base as occurs in twin brackets7. However, in the present study it was verified that the twin bracket InVu obtained the highest fracture strength, suggesting that the fabrication method was more determinant to the fracture strength than the winglet configuration of the bracket.
Insertion of the metal channel with either stainless steel (Clarity) or gold (Luxi II) had no influence on the fracture strength during torque simulation, and presented the lowest values. Ceramic reinforcement on the semi-twin Mystique brackets had no influence on the fracture strength either, when compared with the twin ceramic brackets.
In this study the 0.019"x 0.025" stainless steel arch was used because it is the most commonly used type of arch by orthodontists during the stages of control and torque incorporation in orthodontic treatment.
The variation in force necessary for the orthodontic movement of inclination (torque) of the maxillary central incisor is high, starting with a minimum of 941 g·mm up to a maximum of 3500 g·mm, has been reported by Nikolai10. The fracture strength means during the torque movements in this study ranged from 4885.8 g·mm (Luxi II) to 8113.2 g·mm (InVu). Therefore, after simulation of torque, the brackets evaluated in this study presented higher fracture strength than that necessary for torque movement reported in the literature. Thus, they showed the strength to bear the forces required for dental movement without fracturing. Nishio11 also reported that the ceramic brackets Clarity, Luxi II and 600 Transcend (3M Unitek, Monrovia, CA, USA) bear the force necessary for movement of torque and did not find no correlation between the dimensions of the brackets and fracture resistance. Ceramic bracket fracture at the moment of torque may therefore be due to the excess of force incorporated during torsion of the archwire, and not due to lack of bracket strength, this being an important parameter for the prevention of undesirable effects, such as dental resorptions, for example, commonly found in these types of movements.
In the present study, the fracture site of the bracket and the arch angulation were not verified during the mechanical test, and thus complementary studies are necessary.
It may be concluded that the traditional twin ceramic bracket InVu (TP Orthodontics) presented the highest fracture strength during torque simulation in comparison with the Mistyque, Clarity and Luxi II brackets, probably due to the method of fabrication.
References
1. Maltagliati LA, Feres R, Figueiredo MA, Siqueira DF. Braquetes estéticos – considerações clínicas. Rev Clin Ortod Dent Press. 2006; 5: 89-95.
2. Faltermeier A, Behr M, Müssig D. In vitro colour stability of aesthetic brackets. Eur J Orthod. 2007; 29: 354-8.
3. Viazis AD, Delong R, Bevis RR, Douglas WH, Speidel TM. Enamel surface abrasion from ceramic orthodontic brackets: a special case report. Am J Orthod Dentofacial Orthop. 1989; 96: 514-8.
4. Viazis AD, Cavanaugh G, Bevis RR. Bond strength of ceramic brackets under shear stress: an in vitro report. Am J Orthod Dentofacial Orthop. 1990; 98: 214-21.
5. Karamouzos A, Athanasiou AE, Papadopoulos MA. Clinical characteristics and properties of ceramic brackets: A comprehensive review. Am J Orthod Dentofacial Orthop. 1997; 112: 34-40.
6. Viazis AD, Chabot KA, Kucheria CS. Scanning electron microscope (SEM) evaluation of clinical failures of single crystal ceramic brackets. Am J Orthod Dentofacial Orthop. 1993; 103: 537-44.
7. Johnson G, Walker MP, Kula K. Fracture strength of ceramic bracket tie wings subjected to tension. Angle Orthod. 2005; 75: 95-100.
8. Aknin PC, Nanda RS, Duncanson MGJR, Currier GF, Sinha PK. Fracture strength of ceramic brackets during arch wire torsion. Am J Orthod Dentofacial Orthop. 1996; 109: 22-7.
9. Holt MH, Nanda RS, Duncanson MGJR. Fracture resistance of ceramic brackets during arch wire torsion. Am J Orthod Dentofacial Orthop. 1991; 99: 287-93.
10. Nikolai RJ. Bioengineering analysis of orthodontic mechanics: Lea & Febiger, Philadelphia; 1985. p.299-305.
11. Nishio C, Mendes AM, Almeida MA, Tanaka E, Tanne K, Elias CN. Evaluation of esthetic brackets' resistance to torsional forces from the archwire. Am J Orthod Dentofacial Orthop. 2009; 135: 42-8.
12. Lohbauer U, Amberger G, Quinn GD, Scherrer SS. Fractographic analysis of a dental zirconia framework: a case study on design issues. J Mech Behav Biomed Mater. 2010; 3: 623-9.
13. Scoot GEJ. Fracture toughness and surface cracks – the key to understanding ceramic brackets. Angle Orthod. 1988; 58: 5-8.
14. Russel JS. Aesthetic orthodontic brackets. J Orthod. 2005; 32: 146-63.
15. Gibbs SL. Clinical performance of ceramic brackets: a survey of the British orthodontist's experience. Br J Orthod. 1992; 19: 191-7.
16. TP Orthodontics. Available from: www.invubrackets.com. 17. Anuavice KJ. Phillips science of dental materials. Philadelphia, Penn: Saunders; 2003. p.85-6.
 Correspondence:
Correspondence:
Heloísa Cristina Valdrigh
Centro Universitário Hermínio Ometto - Uniararas
Departamento de Ortodontia Av. Dr. Maximiliano Baruto, 500
Jardim Universitário Araras - SP - Brasil - CEP 13607-339
Phone: +55 19 3543 1474 Fax: +55 19 3543 1412
E-mail: vedovelloorto@terra.com.br
Received for publication: April 02, 2011
Accepted: July 13, 2011